NHS performance and waiting times
Priorities for the new government
NHS performance and waiting times
22 November 2019
About 11 mins to read

Key points
This long read was produced during the 2019 General Election.
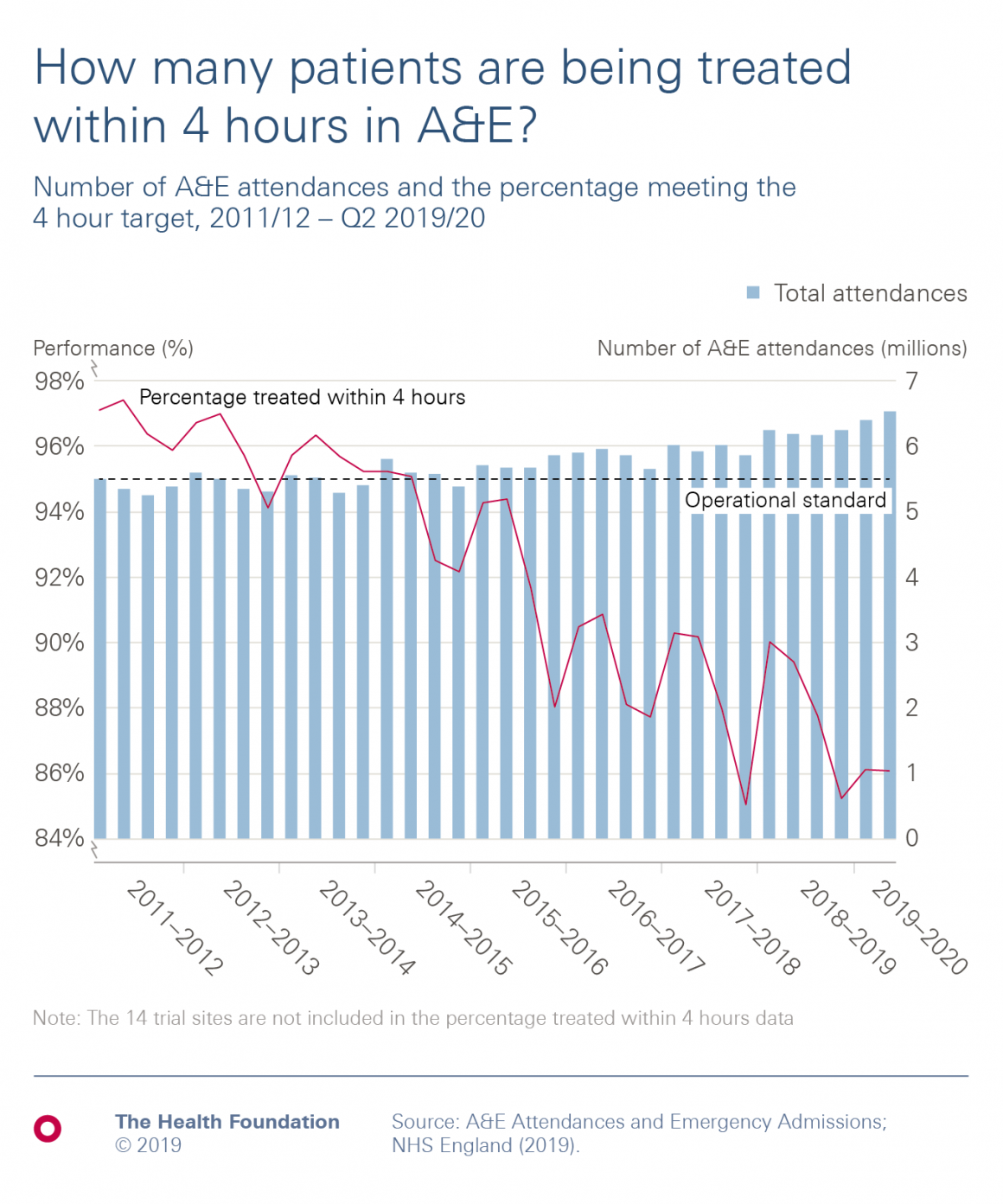
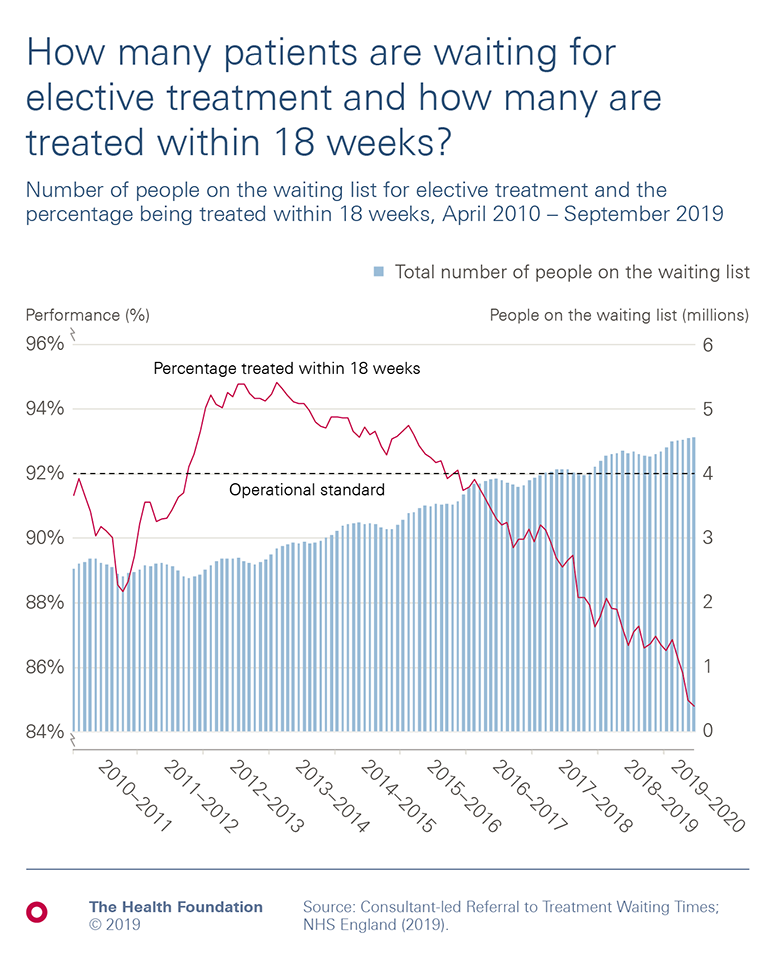
- Essential parts of the NHS in England are experiencing the worst performance against waiting times targets since the targets were set. This includes the highest proportion of people waiting more than four hours in A&E departments since 2004, and the highest proportion of people waiting over 18 weeks for non-urgent (but essential) hospital treatment since 2008.
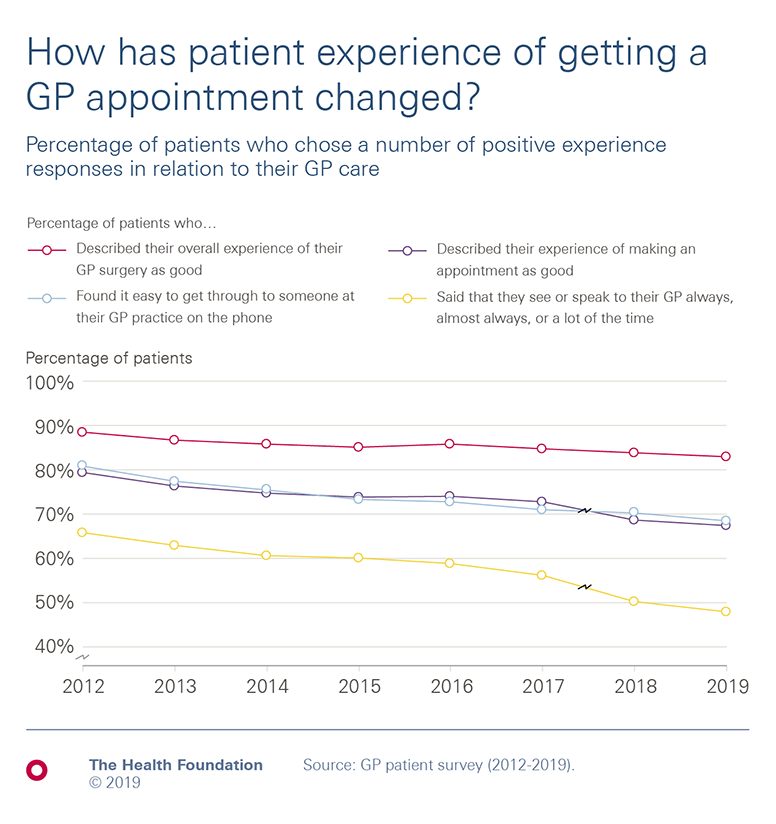
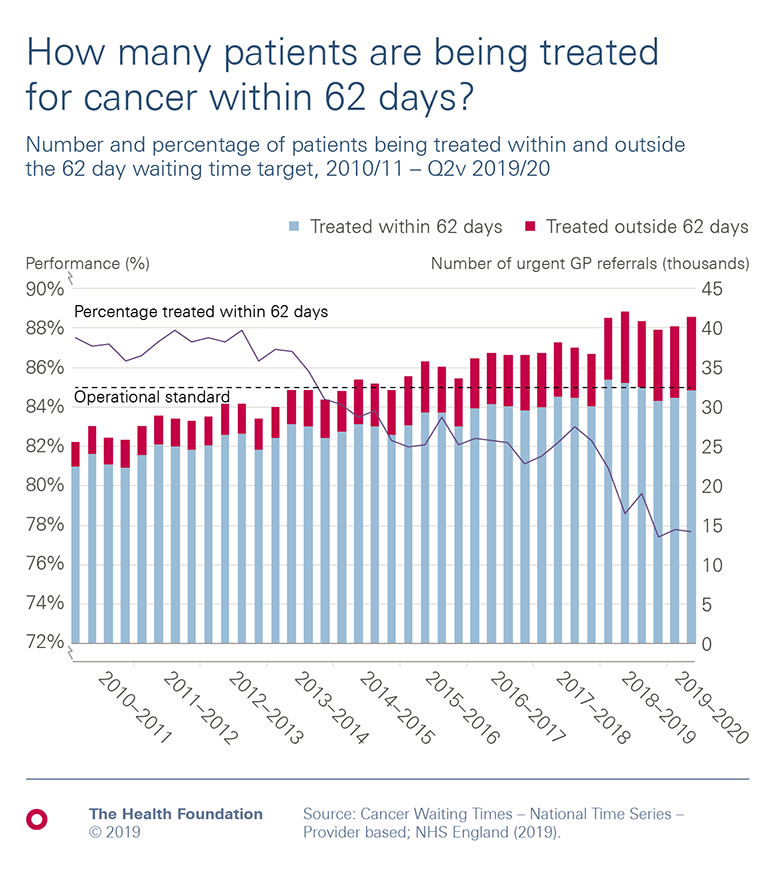
- The target for treating cancer patients within 62 days of urgent GP referral has not been met for over 5 years, and survey evidence suggests more people are experiencing lengthening delays in getting GP appointments.
- Longer waits are a symptom of more people needing treatment than the NHS has the capacity to deliver. This reflects a decade of much lower than average funding growth for the NHS and workforce shortages, coupled with growing and changing population health needs. These pressures are exacerbated by cuts to social care and public health budgets, which make it harder to keep people healthy outside hospitals.
- It will take sustained investment in the NHS and social care to reverse lengthening waits. This will include filling existing staff vacancies and growing the workforce, investment in buildings and equipment, and stabilising the social care sector.
- If the NHS is to achieve its long-term vision of a service that can prevent ill-health, better manage long-term conditions, and treat people earlier, NHS staff will need time, space and skills to make change at all levels of the health and care system.
NHS performance and waiting times
Work with us
We look for talented and passionate individuals as everyone at the Health Foundation has an important role to play.
View current vacanciesThe Q community
Q is an initiative connecting people with improvement expertise across the UK.
Find out more