How are total triage and remote consultation changing the use of emergency care?
3 December 2020
Key points
- The rapid response to the coronavirus (COVID-19) pandemic has engendered a global shift in practice across a variety of health care settings. During the early stages of the pandemic in March 2020, NHS England advised all GPs to move to ‘total triage’ (where every patient contacting the practice is triaged before an appointment) and remote consultations (consultations by telephone, video or online).
- It has been argued that total triage and remote consultations could reduce visits to A&E as a result of faster and improved access to advice, support and treatment from primary care. Conversely, changing the way primary care is accessed might make access more difficult for some patient groups making them more likely to seek care at A&E.
- Here, we look at how total triage and remote consultations are changing the use of emergency care. We compare the demand for emergency care from patients registered at ‘early adopter’ GP practices, which adopted total triage and remote consultations prior to mid-2019, with the demand from patients registered at ‘late adopter’ GP practices, which only started to use total triage and remote consultations after the pandemic began in March 2020.
- During 2019, when only the early adopters were using total triage and remote consultations, there were an average of 3% fewer A&E visits in patients registered at early adopters compared with patients registered at late adopters. During this time there was no difference in emergency admissions between the two groups.
- During the pandemic, the rates of A&E visits and emergency hospital admissions fell among the early adopters by up to 51% and 35% respectively, compared with the same period in 2019. However, these reductions are in line with national trends and are probably related to a reluctance to access care for fear of being infected with the virus, or feeling a burden on the NHS, rather than any impact of digital-first primary care.
- These results provide early evidence that total triage and remote consultations may have the potential to reduce A&E visits. However, we cannot be sure of the precise mechanisms underlying these differences.
- Our analysis has some limitations. We only looked at a single provider of software for total triage and remote consultations and results are not generalisable. In addition, the dramatic changes in the way NHS services now operate as a result of COVID-19 mean that these findings may not be directly applicable as we go forward. More time for recovery, as well as analysis of a more representative set of GP practices, is required for firm conclusions.
Introduction
The rapid response to the COVID-19 pandemic has engendered a global shift in practice across a variety of health care settings, including the UK. During the early stages of the pandemic in March 2020, NHS England advised all GPs to move to ‘total triage’ (where every patient contacting the practice is triaged before an appointment) and remote consultations (consultations by telephone, video or online). A July 2020 RCGP survey reported that more than 88% of UK practices are now equipped for online or video consultations, compared with just 5% pre-pandemic. In the 4 weeks to 18 October 2020, less than 40% of GP consultations were delivered face-to-face in comparison with 73% in the same period in 2019.
Digital-first primary care, where patients use digital and online tools for faster and improved access to advice, support and treatment, plays a key part in the NHS long term plan. As part of this, total triage and remote consultations are designed to improve access for patients and reduce workload pressures on GPs. However, GPs have urged caution and more research is required to understand the impact of different aspects of digital-first primary care on patients, the workforce and the wider health and care system.
In this analysis, as part of an exploration of the impact of digital-first primary care on the wider health and care system, we look at how total triage and remote consultations are changing the use of emergency care. We explore how the demand for emergency care varies between patients registered at practices using total triage and remote consultations, and those patients registered at practices that are not using these approaches. We can only realistically do this before the pandemic began as afterwards the majority of practices started adopting total triage and remote consultations. After the pandemic began in March 2020, we focus on the early adopters and describe the demand for emergency care for patients registered at these practices.
Understanding how the demand for emergency care varied between these different types of practices before the pandemic began, as well as how the early adopters – who by 2020 had been using total triage and remote consultations for some time – coped in 2020, provides insights into the potential advantages and challenges of these approaches.
Why might total triage and remote consultations affect emergency care?
Approximately 15% of A&E presentations are estimated to be for non-urgent conditions that could be managed in primary care. It has been argued that faster and improved access to advice, support and treatment from primary care via total triage and remote consultations could contribute to reduced presentations for non-urgent conditions at A&E and other NHS services.
Conversely, the use of total ‘digital’ triage, where patients are triaged using an online consultation system prior to submitting a request to the GP practice, may increase A&E visits as a result of over-cautious implementation of ‘red flags’. However, similar concerns expressed when NHS 111 was first rolled out were shown to be unfounded. In addition, when the experience of access to primary care is difficult, patients are more likely to seek care at A&E. By attempting to meet the needs of the majority, appointment systems may become more complex and difficult to navigate. Without simplification or effective communication, this could inadvertently disadvantage some patient groups – often those already experiencing greater obstacles to accessing care.
What data did we look at?
We examined 209 practices that started using askmyGP, an NHS-approved digital platform, from August 2018 onwards. askmyGP offers total digital triage and remote consultation to practices across the UK. Patients make contact via a link from the practice website. Non-digital users are taken through the same process by practice staff over the phone. Clinicians and staff then prioritise and deliver care by face-to-face or by telephone, home visit, online or video consultation, according to patient preference and needs.
We obtained data on visits to Type 1 (major consultant led 24-hour services) and Type 3 (doctor or nurse led A&E/minor injury) A&E departments for patients registered at these practices and all other GP practices in England open between September 2016 and July 2020.
Our method relied on identifying 19 of the 209 askmyGP practices as ‘early adopters’ – those using askmyGP for all consultation requests before mid-2019, well before the coronavirus pandemic began. We also identified 133 ‘late adopters’ – those adopting askmyGP for any consultation requests only after the pandemic began. We then compared the demand for emergency care in these two groups of practices. To assess whether any observed differences were the result of chance alone, we ran a difference-in-differences analysis which adjusted for any differences in key demographic, socioeconomic, geographic and administrative characteristics between these two groups of practices.
We also describe how demand for emergency care at these askmyGP practices compares with average demand across all GP practices in England, only a small proportion of which are assumed to have been using digital platforms before the pandemic began.
The 152 early and late adopter askmyGP practices are broadly representative of national trends in terms of number, sex and education of patients. However, 20% of patients are older than 65 years compared with 18% nationally, only 7% live in the most deprived fifth of areas and only 9% have black and minority ethnicity and compared to 16% nationally. 58% of practices lay in urban areas, 24% in small towns and the remaining 18% in rural areas, compared with 46%, 40% and 13% nationally, respectively.
What happened prior to the pandemic?
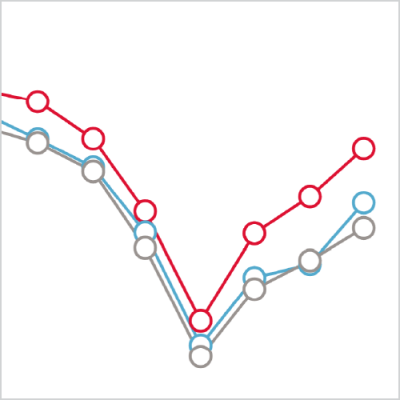
Before the early adopters started using askmyGP prior to September 2018, there were no obvious differences in the average rate of A&E visits between the early adopters (blue lines) and the late adopters (red lines). From September 2018 onwards, as the early adopters began using askmyGP, the rate of A&E visits diverged between the two groups. During 2019, the early adopters had 8.0 (95% confidence interval [CI], 1.5 to 14.5; p=0.016) fewer A&E visits per 10,000 patients per month than the late adopters. This is equivalent to a relative reduction of 3.4% and a total of 1,563 fewer visits to A&E (95% CI 293 to 2,833). The p value represents the probability of seeing this difference by chance alone. Since it is less than 0.05, we are more than 95% confident this is not the result of chance and that the impacts are real, notwithstanding the relatively small sample size.
In contrast to the pattern seen for the average rate of A&E visits, there were no discernible differences in the average rate of emergency admissions between early and late adopters at any time between September 2016 and July 2020. A test for a difference in rates during 2019, when the early adopters had started using askmyGP and the late adopters had not, was not significant (p value = 0.16).
The average rates of A&E visits and emergency admissions at the askmyGP practices are consistently higher than the national average (grey lines) for practices in England throughout. This reflects that these practices are not a fully representative sample of GP practices in England. In particular, they are over representative of patients older than 65 years who are more likely to seek care, and who live in urban areas where rates of A&E visits are likely to be higher than in rural areas.
What happened during the pandemic?
During the pandemic from March to July 2020, the early adopters experienced rapid decreases in the average monthly rates of A&E attendance and emergency admissions. For example, compared with the same period in 2019, the early adopters had 51% and 33% fewer A&E visits and emergency admissions in April 2020 respectively. During the pandemic, the average rates of A&E attendance and emergency admissions also dropped nationally and in the late adopters. Since the NHS encouraged all practices to adopt total triage during the pandemic it is not possible to make robust comparisons between the early and late adopters according to whether they are or are not using these methods at this time.
However, the reduced rates observed in the early adopters during the pandemic are in line with national trends and probably related to a reluctance to access care for fear of being infected with the virus, or feeling a burden on the NHS, rather than any impact of digital-first primary care. From 25 April 2020, in response to an information campaign launched by the NHS which encouraged people to seek the care and treatment they needed, the demand for care increased and successive months indicate a return towards 2019 rates.
Discussion
Our analysis of hospital activity in 2019 (before the pandemic) suggests that adoption of the askmyGP model of total triage and remote consultation was associated with fewer A&E visits. However, our analysis does have some limitations. We only looked at a single provider of software for total triage and remote consultation and practices are skewed towards patients living in urban areas, and with low proportions of black and minority ethnic people. Results will not necessarily be generalisable to other providers, or the general population.
This evidence was also gleaned in 2019, before the COVID-19 pandemic started. During the pandemic, the drop in the rates of A&E visits and emergency admissions we see here is in line with that reported elsewhere. These drops are the result of a complex set of interactions during the COVID-19 pandemic with three main drivers: changes in the way NHS services operate, changes in patient behaviours, and changes in the health need of the population. These dramatic shifts mean that the digital effect we observed pre-COVID-19 may not be applicable as we go forward, and more time is required to reach firm conclusions. In spite of these limitations, our findings offer a baseline estimate of the potential impact of digitalisation on emergency care.
More work is required to determine the precise mechanism of how working digitally causes fewer A&E visits and the resulting impacts on quality of care and patient inequalities. Decreases in A&E visits may be due to faster and improved access to care as a result of efficient triage and perhaps the convenience of round the clock submissions for consultations. This may make it easier for some patients to access care that they previously could not. However, this could be offset by a potential increase in A&E visits due to some patients experiencing greater difficulty in accessing care.
Patient experience of care is also an important factor in whether patients are likely to seek care at A&E. Rollout of technological capability on its own will not work effectively unless health and care staff are supported to develop the skills and capabilities to use it well. For example, empathy and person-centred communication is a key quality consideration for remote consultation and we cannot assume that staff automatically have the skills for this (as the majority have been trained in the face-to-face delivery of services).
Salvie Ltd. has kindly shared data with us for research and evaluation purposes. If the NHS wants to continue to learn from studies such as this, it is important that health care providers, commissioners and evaluators work together to create an environment that allows access to better quality and more meaningful data. We are also working on data access agreements with other digital providers aiming to bring together public and private data to explore the impacts of different models, and other aspects of digital-first primary care, on a variety of different outcomes. Please get in touch if you are interested in sharing your data for our research.
The Health Foundation is also funding other research on remote consultations to understand how COVID-19 has impacted the scaling-up of video consultations. Those implementing digital-first care can connect with others doing this work to share practical learning, tips and challenges through the Q Community.
Acknowledgements
We thank Salvie Ltd. for sharing data for this analysis.
Further reading
Work with us
We look for talented and passionate individuals as everyone at the Health Foundation has an important role to play.
View current vacanciesThe Q community
Q is an initiative connecting people with improvement expertise across the UK.
Find out more

