How reliant is the NHS in England on international nurse recruitment?
12 June 2023
-
Registered nurse vacancies account for over a third of all full-time equivalent NHS staff vacancies in England. Compared with many other OECD countries, the UK relies heavily on internationally recruited nurses to fill funded posts.
-
Recent Nursing and Midwifery Council (NMC) data underline this reliance on international nurses, showing that the annual number of new nurse registrants from outside the European Economic Area has increased significantly and in 2022/23 reached the highest level since records began in 1990/91.
-
In 2022/23, more than 40% of all new nurses registered with the NMC (domestic and international) came from low and lower middle income countries (using World Bank classification), up from 10% in 2018.
-
Last year, more than 6,000 new nurses registered in the UK came from so-called ‘red list’ countries – highlighted by the World Health Organization as being most at risk of not achieving universal health coverage because of health workforce shortfalls.
-
Migrant workers have long been an important part of the UK’s health and care workforce, and international recruitment is vital to addressing staffing shortages in the NHS. But recruitment must be ethical and sustainable, recognising global shortfalls in workers.
-
For longstanding shortages in the nursing workforce to be addressed effectively, it is vital for government’s long-term NHS workforce plan to be comprehensive and fully funded. Alongside this, a long-term plan to reform pay, training and conditions in social care is long overdue.
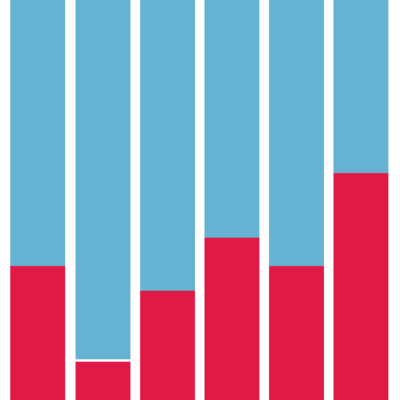
Figure 1
Registered nurses are the most prominent occupation in terms of workforce shortages in the NHS in England. Although they make up around 1 in 4 full-time equivalent (FTE) staff working in NHS hospitals and community services, they account for over a third of FTE vacancies (NHS trusts registered around 40,000 FTE registered nursing vacancies in the quarter to March 2023).
OECD data show that the proportion of UK-based nurses who are foreign trained (nearly 18% in 2021) is well above that in many comparable OECD countries. The health and care sectors in the UK could not function without these internationally trained staff. However, international recruitment is no panacea for all NHS workforce shortages, as international recruits are unequally distributed across regions and care settings. For example, only 3% of new international NMC nurse registrants in 2021/22 were registered in mental health, learning disabilities or children’s nursing – and the UK faces growing competition from other OECD countries for a finite pool of international recruits.
A long-term and growing reliance on international recruitment can result in reduced incentives to invest in domestic education, and there are also ethical concerns around recruiting staff from lower income countries also facing pressing workforce shortfalls. It is therefore important to understand how the extent to which the NHS relies on nurses trained in other countries has changed over time.
Data from the Nursing and Midwifery Council (NMC) on the country of training for new NMC registrants provide useful insights. Between 1990/91 and 2022/23, nurses trained outside the UK have accounted for between 10% and 53% of the overall annual number of new NMC registrants each year. NMC data, released in May 2023, show that over 24,000 of new registrants in 2022/23 were trained outside the UK, nearly half the overall total of all new registrants (Figure 1).
The mix of countries training new NMC international nurse registrants has changed over time. In the latter half of the 1990s and the early 2000s, there was a rapid increase in non-European Economic Area (EEA) international nurse recruitment, notably from the Philippines and India. Subsequently, the period from 2010 to 2016 saw a switch to rapid growth in the recruitment of nurses trained in EEA countries. In the years since 2016, which saw the Brexit vote and new English language test requirements being introduced for nurses, international nurse recruitment from EEA countries has dropped markedly. At the same time, there was a substantial increase in new nurse registrants from non-EEA countries (Figure 2). The NMC’s data release for 2022/23 shows that the number of new registrants trained in non-EEA countries has reached a 32-year high (around 24,300).
Figure 2
In order to assess the mix of low, middle and higher income countries for these UK registrants, we analysed the income level of source countries using the World Bank Atlas classification approach. This compares gross national income per head across countries converted to US dollars to account for exchange rate fluctuations. Our analysis reveals a substantial increase in numbers and the proportion of all new NMC registrants trained in low and lower middle income countries (LI and LMICs) over the past 5 years, from 10% (around 2,500) in 2017/18 to 43% (around 22,700) in 2022/23 (Figure 3).
Three countries account for a substantial majority (80–90%) of all new non-EEA registrants: India, the Philippines and Nigeria.
Figure 3
In 2010, the World Health Organization (WHO) Global Code of Practice on the International Recruitment of Health Personnel set out a framework for ethical international recruitment of health care workers. The Code is increasingly important in light of growing concerns over the ethics of high-income countries plugging domestic workforce shortages at the expense of health workforces in lower income countries.
More recently, the WHO published the health workforce support and safeguards list. This identifies those countries, such as Nigeria, Ghana and Zimbabwe, most at risk of not achieving universal health coverage because of health workforce shortfalls, measured by low numbers of doctors, nurses and midwives per capita.
The UK government Code of practice for the international recruitment of health and social care personnel in England outlines that there should be no active recruitment from these so-called ‘red list’ countries – though direct applications by individual health and social care personnel are not prevented. Since 2019/20, there has been a tenfold increase in the number of new NMC registrants from red list countries (Figure 4). Over 1 in 10 (12%) new NMC registrants in 2022/23 were trained in red list countries (just over 6,000), with over half of these trained in Nigeria. Ghana has also registered a substantial increase in the number of new NMC registrants over the past 5 years, from 19 in 2017/18 to 1,263 in 2022/23.
Figure 4
Discussion
As it normally takes 3 years to train a registered nurse in the UK, active international recruitment has long been regarded as a quick fix to addressing the longstanding NHS nurse shortfall because it can take months rather than years. It is also cheaper as the cost of training is borne by the nurses themselves or governments of other countries. OECD data suggest that the number of nurses trained per capita in the UK in 2020 was substantially lower than in many comparable countries, such as Australia and the US.
It is important for effective national nurse workforce policy planning to align the numbers of nurses coming into the workforce from domestic and international sources, and to be able to monitor and assess how international numbers might impact on UK domestic supply capacity. In addition, there is a need to be able to assess more clearly if the NHS is complying with its own ethical recruitment guidelines on lower resource and red list countries.
Nursing shortages across the NHS and social care are a huge risk to the post-pandemic recovery. It is vital that the government’s promised long-term workforce strategy for the NHS is backed by full funding and with alignment between effective domestic training and effective and ethical international recruitment. Alongside this, a long-term plan to reform pay, training, and conditions in social care, which supports ethical international recruitment, is long overdue.
Further reading
Work with us
We look for talented and passionate individuals as everyone at the Health Foundation has an important role to play.
View current vacanciesThe Q community
Q is an initiative connecting people with improvement expertise across the UK.
Find out more

