Response to the Autumn Budget 2018 Day to day spending on the wider health budget will fall by £1bn in real terms next year
30 October 2018
Anita Charlesworth, Director of Research and Economics for the Health Foundation, said:
‘The NHS was the clear winner in the Chancellor’s budget but there is a big risk that it won’t feel like that in hospitals and GP surgeries over the coming year. Extra funding starts next year and rises to £20.5bn in 2023/24. This money is for front-line NHS services. It excludes wider areas of vital health spending where funding is also desperately needed; public health, workforce training and capital investment.
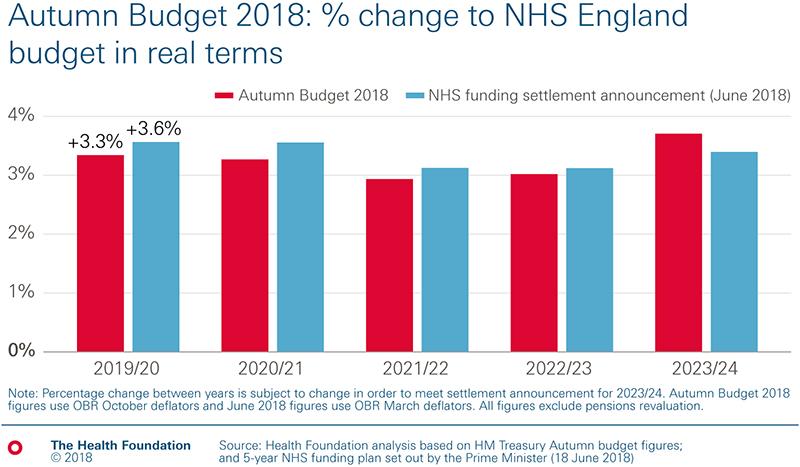
‘The Department of Health and Social Care’s overall budget will therefore increase by just 2.7% in 2019/20 – less than the 3.3% minimum required just to stand still in the face of ever rising demand and cost pressures. On top of this, higher than expected inflation means that unless the Chancellor tops up next year’s NHS England allocation before his spending review, the NHS England budget will increase by 3.3%, which is less than the 3.6% promised by the Prime Minister in the summer. To meet this 3.6% commitment would require an additional £260m in cash terms. The phasing matters as the NHS is overstretched and short of capacity now.
'Day to day spending on the wider health budget which includes funding for doctor and nurse education and training, and public health – and the impact of pensions revaluation – will fall by £1bn in real terms next year. Capital investment budgets are planned to increase. In recent years the department has raided capital funds to support day to day spending. If the government wants to avoid further cuts to education and public health, it will need to shift all of the planned capital growth to day to day resource budgets.
‘The Chancellor’s announcement of a freeze on PFI leaves the health service with a potential £3bn hole in its capital investment budget. This follows major underinvestment in buildings and infrastructure as capital spending in the NHS has fallen by more than 20% in real terms over the last three years.
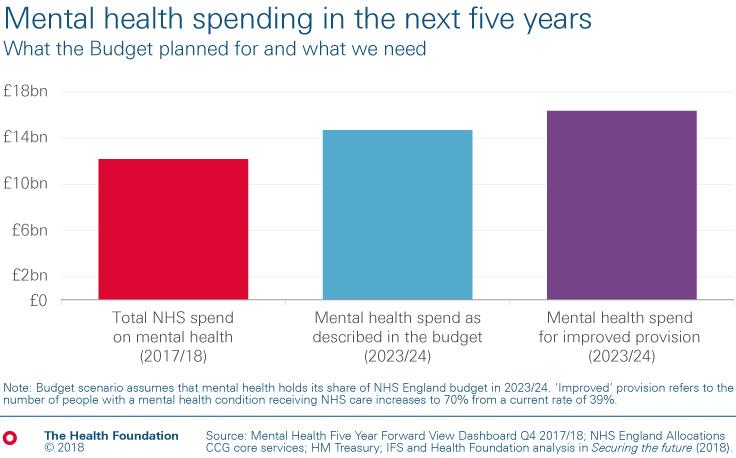
‘Extra investment in mental health services will see funding grow broadly in line with the total health budget but this will mean simply maintaining the status quo which sees just 4 in 10 people who need it receive mental health support. To see some improvement, with provision increasing to 7 in 10, the service would need an extra £1.5bn on top of what the chancellor has announced.
‘Social care will see an estimated 2.9% in real terms increase next year. While welcome, this falls far short of rising pressures of 3.9% per year and offers little scope to address unmet need or improve quality. Drip feeding short-term cash injections is not the way to manage this vital public service. It will not address the manifest unfairness in a system which leaves those in need without help and provides no protection for people from catastrophic care costs.
‘While additional money has been pledged for local authorities to deliver social care services, it is disappointing to see further cuts of £200m to public health services which have already seen reductions of £500m since 2014/15. A decision on future public health funding has been delayed until the 2019 spending review but the Prime Minister has so far only committed to ‘continuing to support public health’. Next year the public health grant will fall in real terms. This is unacceptable and runs counter to the government’s policy emphasis on prevention. An extra £3.2bn is needed per year to restore provision following the damaging cuts of recent years and reallocate funding according to need, ensuring that no local authority is worse off.
‘While NHS front-line services will receive a real terms uplift, the same cannot be said for wider public services that have a direct impact on people’s health. It will be vital that the government addresses this in the forthcoming spending review. Resolution Foundation analysis shows that spending on unprotected public services will continue to fall on a per person basis unless the Chancellor finds extra money for next year’s spending review. This means areas of public spending such as education, which are key to people’s good health, face further reductions.
‘Although cuts to Universal Credit have been reduced, following this budget, welfare payments for low income families will still be cut. The tax changes announced will overwhelmingly benefit higher income households. This matters as poverty is strongly linked to worse health. The outcome of Brexit negotiations will be crucial as it may mean a reduced or increased spending envelope. Spending on the NHS is necessary but far from sufficient to safeguard and improve health.’
Change in health budget, 2018/19 prices*
|
2018/19 |
2019/20 |
2019/20 (real terms) |
Real percentage change |
Real amount change |
|
|
Health budget |
£129.2 |
£135.1 |
£132.7 |
2.7% |
£3.5 |
|
New NHS England budget |
£114.6 |
£120.6 |
£118.4 |
3.3% |
£3.8 |
|
Previous NHS England budget |
£114.6 |
£120.6 |
£118.7 |
3.6% |
£4.1 |
Download the table (PNG) *Using OBR October deflators unless otherwise specified. ‘Total health budget' is total DEL for the Department of Health and Social Care. 'Previous NHS England budget' is as at the Prime Minister's June announcement, using OBR March deflators. The difference is due to increased rates of inflation forecast by the OBR. All figures exclude pensions revaluation.
Media contact
Simon Perry
External Affairs Manager
Simon.Perry@health.org.uk
020 7257 2093
Further reading
Work with us
We look for talented and passionate individuals as everyone at the Health Foundation has an important role to play.
View current vacanciesThe Q community
Q is an initiative connecting people with improvement expertise across the UK.
Find out more