The real cost of a fair adult social care system
29 May 2019
Key Points
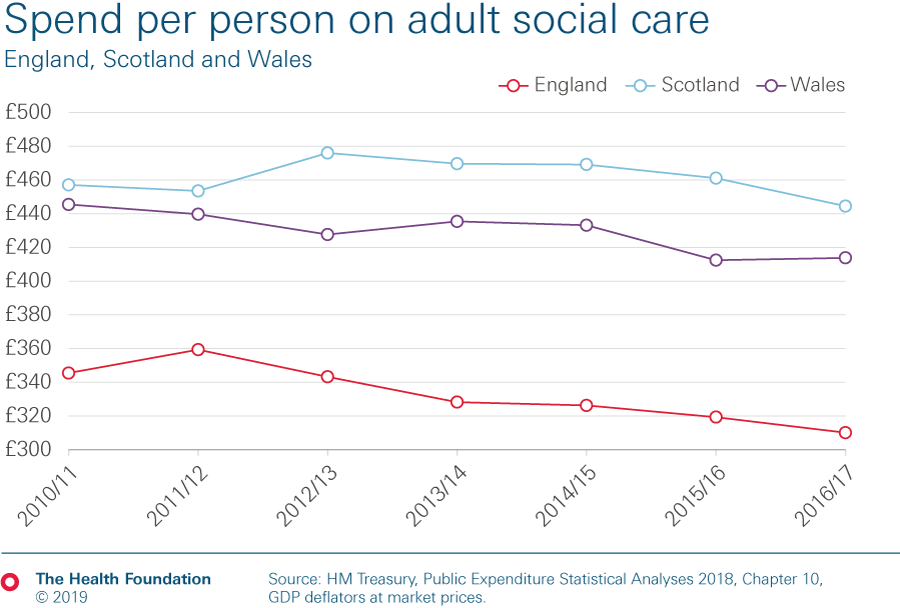
- Government spending on adult social care in England fell from £345 per person in 2010/11 to £310 in 2016/17.
- In 2010/11, adult social care spending per person on was a third lower in England than in Scotland. By 2016/17, the gap had widened to 43%.
- If funding levels in England had grown in line with increasing demand since 2010/11, adult social care funding would have been £6bn higher than actual spending in 2017/18.
- Without additional funding, the money available for adult social care will rise by an annual average rate of 1.4% a year from 2017/18 to 2023/24 – much lower than the rate of increase promised to the NHS of 3.4% a year and demand pressures of 3.6% a year.
- Without additional government funding, there will be a gap between demand pressures and available resources of at least £2.7bn in 2023/24. This is in addition to the £6bn gap which opened up between 2010/11 and 2017/18.
- This gap would be £4.4bn by 2023/24 if social care staff were given a similar pay uplift to the planned increases for NHS workers. Without this, social care will continue to struggle to compete with other sectors, including health care, in recruiting and retaining staff.
Nobel laureate Sir Angus Deaton, famous for documenting declining life expectancy as a result of so-called 'deaths of despair' in the USA, has announced that he will be working with the Institute for Fiscal Studies (IFS) to analyse levels of inequality in the UK.
More than 70 years after the foundation of the modern welfare state, there remain deep injustices and inequalities in the UK. Many who need its protection and support at times of vulnerability, find it falls short. We are rightly proud that the NHS is based on need, not ability to pay. Fear of crippling medical bills, that force people to choose between essentials like heating and health care is rare, in this country.
Free at the point of use health care is as essential today as it was after the Second World War. However, the profound changes in society since the founding of the welfare state mean that while free health care is necessary, it is not sufficient to deliver the ambitions of a state that protects the health and wellbeing of its people.
Increased life expectancy was a major triumph of the twentieth century, but its legacy is some 'wicked' public policy challenges for the twenty-first century. There are many more working-age adults living with long-term conditions. (For example, the average lifespan for someone with Down’s syndrome is now 60, in the early 1980s it was just 25 years.) Increased life expectancy has also resulted in prolonged periods of chronic ill health and frailty at the end of life, as healthy life expectancy has not kept pace with overall improvements in longevity.
We rightly expect that society should ensure that those with long-term conditions are able to live high-quality lives and can continue to contribute to social and economic life with effective support. Furthermore, we recognise that a dignified end chapter of a long life is very important to both the individual and those they love.
Sadly, while we can be proud of our health service, the wider system of support through adult social care is, frankly, shameful. Most people don’t realise how different it is to the NHS; it has a highly restrictive needs test and is strictly means tested. When the system is explained to people, almost everyone agrees it’s inadequate and unfair.
Politicians recognise the problem and for over 30 years have repeatedly promised action. A Royal Commission was set up under the Blair government. This led to free personal care in Scotland but little change in England. In 2014, Parliament passed legislation to cap the cost of care for older people but then postponed implementation indefinitely. Adult social care also featured prominently in the 2017 general election but two years on, the promised green paper is still nowhere in sight.
Meanwhile the problems in adult social care grow: rising need has not been matched by funding; responsibility has shifted away from the state towards individuals and their families; and there are serious challenges with care home providers facing financial problems. Furthermore, we have a workforce characterised by low pay, poor terms and conditions, and high turnover.
What do we spend on social care now?
In 2010/11, government spent an average of £345 per person in England on adult social care. After a long period of political neglect (in which the means test thresholds have not been increased in line with inflation), this has fallen to £310 per head in 2016/17.
Adult social care funding varies a lot across Great Britain. As the first chart below shows, spending in England was already lower than in Scotland and Wales in 2010/11 – Scotland spent a third more per person than England. By 2016/17, adult social care spending in England had fallen even further behind with Scotland spending 43% more per person than England. While there are differences in the demography and care needs of each country, to put this figure in context, Scotland spent just 8% more on publicly funded health care in the same year.
While the gap in spending per person has widened for publicly funded adult social care, the difference in health care spending per person between the two countries has narrowed over recent years. In 2010/11, Scotland spent £2,404 per person on health care in real terms, £231 (11%) more than England. While health care spending in both countries has grown over the period, England’s spending has grown faster reducing the gap to £173 (8%).
(Note: Health spending is measured as public spending by health 'function', and includes all spending on the NHS in the UK, but excludes administrative costs. It also includes medical research, devolved administrations and local government spending on health.)
The reduction in spending per person has come at a time when the proportion of the population over 85 has grown. The overall population of England increased by 5% between 2010/11 and 2016/17, but the number over 85 rose by over 14%. If funding levels had grown in line with increasing demand since 2010/11, social care funding would have been £5.4bn higher than actual spending in 2016/17, rising to £6bn in 2017/18.
How much funding is required?
Social care funding is complex. Most public funding comes from local authority budgets; through council tax, business rates and the social care precept, but also from additional ringfence pots from the NHS and central government. The precept has allowed local government to increase council tax by up to 3% a year if the revenue raised is spent on adult social care.
Office for Budget Responsibility projections of local government spending power suggest that real terms social care net expenditure could increase from £17.8 bn in 2017/18 to £19.3bn in 2023/24; an average annual increase of 1.4% a year. Increases above this level would require the government to commit to additional central government funding. Without additional funding, adult social care spending would grow at less than half the rate of the increase promised to the NHS of 3.4% a year, and crucially far below rising demand.
The main and most robust source of projections of social care demand come from a model developed by the London School of Economics. These projections show that, with an ageing population and rising levels of disability, funding would need to grow by 3.6% a year to maintain access and quality of care at the levels of 2015/16. Without additional government funding, there would be a gap between spending pressures and available resources of at least £2.7bn in 2023/24.
Problems with provision
Meeting rising demand is a key challenge for the adult social care system, but not the only one. There is growing evidence of considerable problems with the provision of social care. While most care is good (the Care Quality Commission rate 4 out of 5 providers of home and residential care as good or outstanding), some is not.
There is growing anxiety about the viability of the sector going forward. The government’s Competition and Markets Authority undertook a review of residential and nursing homes for older people in 2017 and concluded that the amounts local authorities are able to pay towards someone’s care are below the full cost of delivering care. Local authorities are increasingly reporting that providers are handing back contracts deemed unviable. The challenges facing providers is well illustrated by the recent news that one of the country's largest care home groups, Four Seasons Health Care, has gone into administration.
The workforce challenge
Social care is a service and as such, its workforce is a key determinant of both quality and cost. Social care is largely an unregulated and unregistered profession in England. Around two-thirds of staff are paid at the minimum wage, many are on zero hours contracts, there is a significant reliance on staff recruited overseas, and turnover is high.
Our 2019 report Closing the gap with The King’s Fund and Nuffield Trust highlighted that rising demand combined with planned changes to make international recruitment more difficult, low unemployment across the economy, and competition for the same pool of potential workers from other sectors (such as the NHS) will compound these problems. These will add to funding pressures.
The NHS has recently agreed a new pay deal for over one million workers. This includes health care assistants and other support workers, who often have the same qualifications and prior experience as those working in social care.
There is a 7% gap between the pay rates for adult social care nurses, and the rates available for nurses in the NHS. Over the next few years, this will rise further with basic pay for NHS nurses starting in 2017/18 increasing by up to 22%, including pay progression. For care workers in the adult social care sector, average full-time equivalent pay in 2017/18 was £16,000. A similar role working to provide support to doctors and nurses in the NHS would pay a fifth higher (£19,300).
There are just over 40,000 nurses working in adult social care but almost a third are estimated to have left their role within the past 12 months.
This is unlikely to be sustainable. Our estimate suggests that, once you map current social care staff to equivalent current pay rates in the NHS, the funding would need to increase by around £1.8bn. This would mean that the gap between cost and demand pressures, and local authority spending power, would be £4.4bn by 2023/24. While this is a significant additional cost, it is hard to see how social care providers can recruit and retain staff at current pay rates when salaries will be higher in competitor labour markets.
An additional £4.4bn would see spending rise by 5.2% a year between 2018/19 and 2023/24. This is a substantial increase in funding.
To put this in perspective, our second chart below shows that if England wanted to provide the same access and quality of publicly funded adult social care as in 2010/11, then the government would need to provide an extra £10bn for local authorities. This is on top of the expected rise in their spending power, based on expected council tax and business rate receipts.
The balance in responsibility
None of this tackles the issue at the heart of the Sutherland Commission of 1999; the balance in responsibility between the individual and the state. The funding increases outlined above are focused on ensuring access and quality of care under the current system.
But reforming the funding system so that the state protects more people from the catastrophic costs associated with paying for their own care would add further to the bill. Implementing the cap on care costs which formed part of the 2014 Care Act would add at least £2.8 billion to the annual cost of adult social care in 2020/21 (with the exact amount dependant on the level of the cap). Our 2018 report with The King’s Fund, Fork in the road, estimates that moving to free personal care along the lines of the Scottish system would add £7 billion in 2020/21.
Perhaps in this context it is not surprising that the social care green paper is still 'forthcoming'. While this may be understandable, and the decisions involved very difficult, the tragedy is that it is individuals and their families who suffer at times of greater need. This part of our welfare state is desperately overdue for serious reform.
Anita Charlesworth (@AnitaCTHF) is the Director of Research and Economics, and Toby Watt (@TLSWatt) is Senior Economist, at the Health Foundation.
Notes:
- All expenditure figures are in 2019/20 prices.
- Pay pressure figures supplied have been rounded up, so totals may not sum.
Further reading
Further reading
Work with us
We look for talented and passionate individuals as everyone at the Health Foundation has an important role to play.
View current vacanciesThe Q community
Q is an initiative connecting people with improvement expertise across the UK.
Find out more