Lower paid NHS and social care staff turnover What occupations do the NHS and adult social care compete with for lower paid roles?
2 November 2022
Key points
- After 2.5 years of COVID-19 and with inflation rising, NHS and social care employers are facing severe recruitment and retention challenges, with vacancies well above pre-pandemic highs. Both sectors rely on many staff who, although often highly skilled, do not have formal qualifications and earn below average UK wages. Understanding the extent to which employers compete with other lower paid occupations for these staff is crucial for workforce planning and pay determination.
- We use Office for National Statistics data to examine the movement of workers into and out of lower paid NHS and adult social care occupations between 2011/12 and 2021/22. We identify the key source occupations (where staff were employed before joining the NHS or social care sector) and destination occupations (where staff moved after leaving the sector).
- In this dataset, around 1 in 4 directly employed NHS employees (across all health care industries) are ‘lower paid’. This is defined as earning up to the top of band 4 of the NHS Agenda for Change hourly pay scale (up to £12.73 per hour in 2021/22 – close to average UK hourly earnings in 2021). By comparison, around 4 in 5 social care employees are ‘lower paid’ by the same measure.
- Lower paid social care workers are employed in a wide range of occupations before joining adult social care. Excluding those in care work to begin with, the most common source occupation is sales and retail assistant, but this only accounts for one in 10 entrants (10%). The next most prominent source occupations are nursing auxiliaries and assistants (9%) and cleaners and domestics (8%).
- The most common destination occupations for lower paid social care staff are nursing and nursing auxiliaries and assistants, accounting for 17% and 11% of departures outside of care work. This indicates that social care often functions as a stepping stone to NHS employment. Policies that aim to address staff shortages only in the NHS could therefore exacerbate vacancies in social care.
- For lower paid NHS staff, social care is a more common source occupation than destination occupation. These staff also had a wide array of external destination occupations, with the most common – miscellaneous administrative roles – accounting for only 11% of the total.
- Our analysis underscores the need for a comprehensive long-term workforce plan for the NHS and social care, accounting for labour market flows across the two sectors and their interaction with the wider economy.
Context
Workforce shortages represent one of the biggest challenges facing the NHS and adult social care in England. In the quarter to June 2022, vacancies in NHS trusts stood at around 132,300 full-time equivalent (FTE), well above pre-pandemic levels. There were around 165,000 vacancies in adult social care in 2021/22, a jump of 52% relative to 2020/21 and well in excess of pre-pandemic highs. With all-economy unemployment touching historically low rates and the pandemic having led to increased workload and burnout pressures for the health and care workforce, there is mounting concern that both the NHS and the adult social care sector (hereafter, social care) are losing staff they desperately need.
In this piece, we take a step back and explore trends in turnover among lower paid NHS and adult social care staff during the past decade (2011/12 to 2021/22). We identify source occupations (where lower paid NHS and social care workers were employed before joining the sector), and destination occupations (where staff moved after leaving the sector). Our analysis complements existing evidence (from Skills for Care and elsewhere) of high rates of turnover within adult social care.
We focus on lower paid staff for two reasons. First, because they play a vital role in health and care provision. Second, the labour market in which they operate is less well understood relative to that for better paid staff groups such as doctors and nurses. The NHS and social care compete for these lower paid workers with other lower paid private sector occupations, whereas the NHS employs a majority of professionally qualified clinical staff such as nurses and doctors. Addressing this knowledge gap is indispensable for resolving longstanding health care staffing shortages, which are likely to worsen over this decade under current policies. Left unaddressed, staff shortages are likely to severely impede efforts to tackle growing NHS backlogs and delays in hospital patient discharge.
For our analysis, we use data for 2011/12 to 2021/22 from the Annual Survey of Hours and Earnings (ASHE), undertaken by the Office for National Statistics. ASHE collects data on earnings from a sample of around 300,000 employee jobs (1% of the population) every year – see the box at the bottom of this page for further detail. We consider lower paid NHS staff and lower paid adult social care staff separately, as movements between the two groups have important implications for workforce policy and planning.
Occupational variation among lower paid staff
Using our definition (all employees whose earnings do not exceed the top of band 4 of the NHS Agenda for Change hourly pay scale), around 1 in 4 NHS employees (in each year from 2011/12 to 2021/22) count as lower paid. This only covers directly employed NHS staff, as our definition cannot capture people who provide services to the NHS through external contractors or outsourcing arrangements.
Among social care employees, the proportion is much higher, ranging from 76% to 82% (around 4 in 5) each year. The results that we present are for those lower paid staff that we can identify in ASHE and may not fully apply to all lower paid staff in both sectors.
There is considerable variation in the proportion of lower paid staff, as defined here, across occupational groups – for example, more than 9 in 10 (92%) care workers and home carers were lower paid between 2011/12 and 2021/22, whereas for social care nurses only around 8% were lower paid.
Flows into and out of lower paid social care and NHS occupations
Where do lower paid adult social care staff come from and move on to?
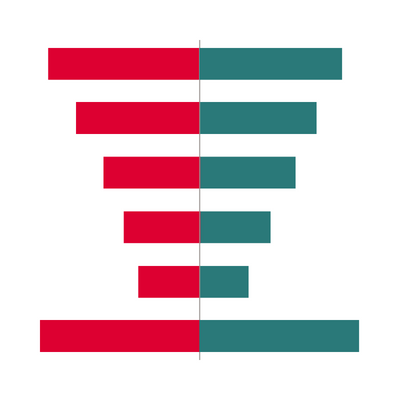
Figure 1 shows the leading source occupations (where people worked before) and destination occupations (where they worked afterwards) for lower paid adult social care staff.
The red bars on the left of Figure 1 show the distribution of source occupations. The largest single source occupation of lower paid social care staff is sales and retail assistants, accounting for 10% of entrants, followed by nursing auxiliaries and assistants at 9%. The next three leading source occupations were cleaners and domestics, kitchen and catering assistants, and miscellaneous administrative roles. It is notable that the 11 top occupations listed only account for around half (51%) of entrants from outside social care, meaning that lower paid social care roles attract workers from a very wide range of industries.
The green bars on the right of Figure 1 show the key destination occupations for lower paid social care staff. In some cases, these employees continued to be lower paid in their destination occupations, but in others they moved on to better paid occupations. The most common destination occupations were nursing auxiliaries and assistants (17%) and nursing (11%). This emphasises that social care is often a stepping stone to employment in the health care sector.
Figure 1
Where do lower paid NHS staff come from and move on to?
Figure 2 shows the leading source and destination occupations for lower paid NHS staff. Again, the source occupations are shown by the red bars on the left. The most common source occupation was care workers or home carers (14% of entrants after excluding those who did not change occupations), again showing how social care acts as a stepping stone to NHS employment. The next most common source occupations were sales and retail assistants (8%) and miscellaneous administrative roles (7%), with a long tail of other occupations accounting for smaller proportions of the total.
The most common destinations outside of the NHS, shown by the green bars, were miscellaneous administrative roles, care workers and home carers, and cleaners and domestics (11%, 7% and 6%). However, almost two thirds of exits (64%) were to a very wide range of other occupations.
Figure 2
What do our findings mean for future workforce planning?
Our analysis provides new insight into flows of workers into and out of NHS and adult social care occupations. We have two principal findings. First, we confirm that social care often acts as a stepping stone to NHS employment, both lower paid and roles that require clinical qualifications. Of staff leaving adult social care for other occupations, 28% were later employed as nurses or nursing auxiliaries and assistants. A much smaller share (7%) move into care work after working for the NHS. This has important policy implications for how best to fill vacancies for lower paid staff in the NHS. Any policies that (further) improve pay and conditions in the NHS relative to social care risk exacerbating social care vacancies.
Second, in line with others’ recent work using the Annual Population Survey, we show that (after excluding those who do not change occupations) the NHS and social care sectors draw staff from a very wide range of occupations. Retail is the most common source, but this accounts for only 10% of total entrants from outside the sector. At least in the ASHE data, the number of people leaving adult social care to go and work in sales and retail is small (3%). However, jobs with large employers – such as retail outlets and supermarkets – may affect pay and conditions in the local labour market, and offer an alternative destination for those working in other lower paid occupations who might have otherwise considered health and social care.
This research is limited to looking at changes in the overall national level occupational mix among lower paid NHS and social care workers during the period from 2011/12 to 2021/22. However, the past decade saw important shifts in the earnings of these staff – particularly in social care – relative to those in occupations such as sales and retail assistants and miscellaneous administrative roles.
In future research, we will examine related issues such as the extent to which our results vary over the time period of interest and by region. We will also explore whether we observe significant links between changes in staff numbers and changes in average hourly pay and the number of hours worked at an occupational level.
Our findings highlight the need for a comprehensive long-term workforce strategy that accounts for how the labour markets for lower paid NHS and social care staff interact with each other and with the wider economy.
Data citation and acknowledgements
Data citation: Office for National Statistics. (2021). Annual Survey of Hours and Earnings, 1997–2021: Secure Access. [data collection]. 19th edition. UK Data Service. SN: 6689, DOI: 10.5255/UKDA-SN-6689-18
Acknowledgements: We would like to thank John Forth and Alex Bryson, whose insights and input have improved this report. We are also grateful to colleagues from the Health Foundation for their reviews and contributions, in particular Lucinda Allen, Anita Charlesworth, Pete Stilwell, Sarah Witts, Kate Addison, Frances Kirk and Tatjana Cvijanovic. Errors or omissions remain the responsibility of the authors alone.
We use data for 2011/12 to 2021/22 from the Annual Survey of Hours and Earnings (ASHE), undertaken by the Office for National Statistics (ONS).
ASHE draws data on earnings from a sample of around 300,000 employee jobs (1% of the population) every year and includes information on respondents’ sex, age, industry (through the 2007 Standard Industrial Classification, SIC 2007), occupation (through the 2010 Standard Occupational Classification, SOC 2010) and region, among other variables. Respondents can be tracked over time and weighted (as in our analysis here) so that they are representative of the population. Despite well-documented limitations due to employer non-response and attrition, ASHE is among the best sources of data for analysis of longer term trends in employee earnings.
We use SIC 2007 to define lower paid health and social care staff in ASHE, with a public–private sector identifier in ASHE serving as a marker for NHS employees within the broader health care industry heading. We define ‘lower paid’ staff to be all employees with hourly pay not exceeding the top of band 4 of the hourly NHS Agenda for Change pay scales in each year from 2011/12 to 2021/22, amounting to a maximum hourly pay rate of £12.73 per hour in 2021/22.
In March 2022, around 2 in 5 (40%) FTE staff in NHS trusts were paid less than £12.73 per hour. This included all health care assistants (HCAs), but not registered nurses in trusts (who typically start at the bottom of band 5). The £12.73 threshold is close to median hourly earnings for all employees in 2021, estimated at £14.10 per hour. It is well above the National Living Wage in 2021/22 (£8.91 per hour) and the median hourly pay of care workers in the independent sector.
Using standard ONS data filters in ASHE, we derive a weighted total of around 1.4 million to 1.6 million NHS employees a year in England, which broadly aligns with NHS Digital estimates of staff directly employed in NHS trusts and general practices. Our definition of social care, however, yields a total of around 500,000 to 600,000 employees a year in England, which is significantly below than Skills for Care’s estimate of 1.5 million. This is attributable to difficulties in fully identifying the social care workforce in ONS data. Using an alternative dataset to ASHE, the Annual Population Survey, or even a different definition in ASHE, leads to varying estimates of workforce size.
As the Migration Advisory Committee stated in their 2022 review of the sector, ASHE is not designed to provide accurate estimates of the size of the workforce, so our analysis cannot claim to represent the entire social care workforce in England. However, the main strength of ASHE over other workforce datasets, such as Skills for Care, is that it is a panel dataset that follows the same people over time across the whole economy. For a subset of lower paid health and care staff who changed occupations, there is information on their occupations and earnings before and after their employment in lower paid health and care roles. We are therefore able to look at the source and destination occupations for these staff.
Further reading
Work with us
We look for talented and passionate individuals as everyone at the Health Foundation has an important role to play.
View current vacanciesThe Q community
Q is an initiative connecting people with improvement expertise across the UK.
Find out more

